Harlequin ichthyosis, impact case.
Keywords:
congenital ichthyosis, harlequin fetus, genodermatosis, harlequin ichthyosis.Abstract
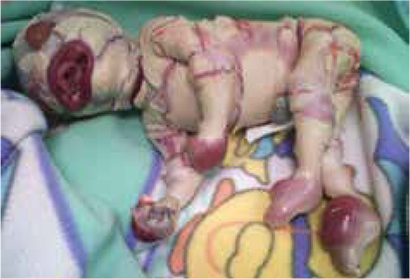
Harlequin ichthyosis is the most severe form of congenital ichthyosis and is often fatal in the perinatal stage because rarely survive more than a week. Hart, described the first case in 1750 and to date there are few published cases. We present a case report of a male newborn with 35 weeks of gestation, whose teenage mother did not attend prenatal care, so the diagnosis was made after birth occurred. He was hospitalized in the neonatal intensive care unit for thermal and electrolyte control and prevention of sepsis of skin origin; however, he died within hours. Although it is a rare entity in clinical practice, the health personnel should know the initial supportive measures to prevent complications and to offer a multidisciplinary approach to these patients.
Author Biographies
Katterine Rojas
Médica pediatra, Universidad Libre, Seccional Cali, Colombia
Jairo Victoria
Dermatòlogo pediatra, docente de posgrado, Universidad Libre, Seccional Cali, Colombia.
Francisco Acosta
Médico pediatra neonatólogo, Universidad del Cauca, Popayán, Colombia.
Edwin Guzmán
Médico ginecólogo y obstetra, Universidad del Cauca, Popayán, Colombia.
References
2. Pongprasit P. Collodion baby: The outcome of long term follow-up. J Med Assoc Thai. 1993;76:17-22.
3. Dyer JA, Spraker M, Williams M. Care of the newborn with ichthyosis. Dermatol Ther. 2013;26:1-15.
4. Pérez A, Pino G. Ictiosis graves del recién nacido: una patología infrecuente. Archivos de Investigación Materno Infantil. 2010;2:56-9.
5. Wright T. The genodermatosis.UpToDate. Fecha de consulta: 25 de agosto de 2015 Disponible en: http://androsma.5gbfree.com/contents/mobipreview.htm?24/0/24586?source=see_link
6. Akiyama M, Sugiyama Y, Sakai K, McMillan JR, MakiGoto M, Arita K, et al. Mutations in lipid transporter ABCA12 in harlequin ichthyosis and functional recovery by corrective gene transfer. J Clin Invest. 2005;115:1777-84.
7. Rodríguez L, Ginarte M, Vega A, Toribio J. Ictiosis congénitas autosómicas recesivas. Actas Dermosifiliogr. 2013;104:270-84.
8. Ortiz-Brugués A. Revisión ictiosis arlequín. Piel. 2013;28:583-90.
9. Vahlquist A, Blockhuys S, Steijlen P, van Rossem K, Didona B, Blanco D, et al. Oral liarozole in the treatment of patients with moderate/severe lamellar ichthyosis: Results of a randomized, double-blind, multinational, placebo-controlled phase II/III trial. Br J Dermatol. 2014;170:173-81.
10. Ávila GA, Montoya M, Bustillo MC, Carrasco DA, Rodríguez C, Carranza N. Ictiosis arlequín: reporte de un caso en honduras y revisión de la literatura. Rev Méd Hondur. 2011;79:199-202.
How to Cite
Downloads
Downloads
Published
How to Cite
Issue
Section
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |






