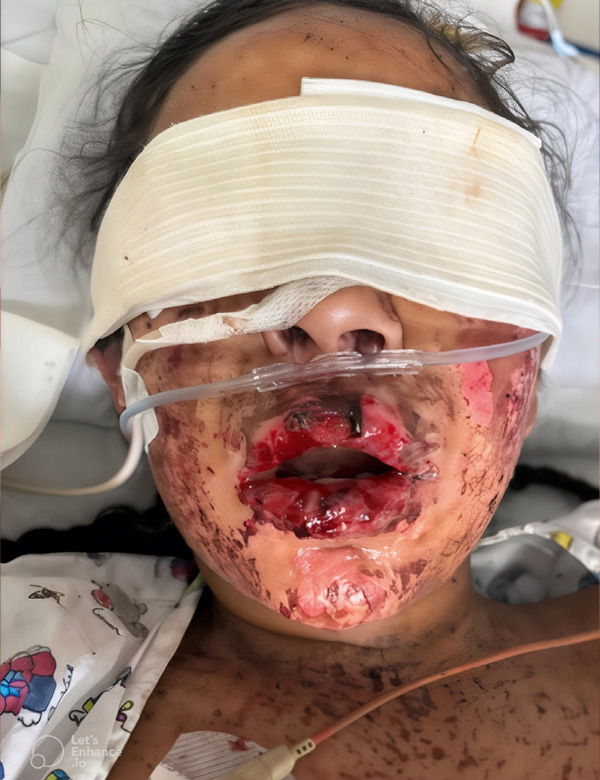
Drug-induced toxic epidermal necrolysis in a pediatric patient: case report and literature review
DOI:
https://doi.org/10.29176/30284163.2077Keywords:
Antibiotic, Childhood, Epidermal necrolyses toxic, Stevens-Johnson syndromeAbstract
Toxicodermias are adverse reactions in the skin caused by medications. Their diagnosis is based on the clinical history and the findings on physical examination, considering that a single medication can present different cutaneous manifestations. Toxicodermias can be classified into non-severe and severe, such as angioedema, Stevens-Johnson syndrome (SJS) / toxic epidermal necrolysis (TEN), among others, which are differentiated by their clinical manifestations, possible sequelae, as well as by their latency period. Mortality varies according to each clinical presentation: for SJS it is 5%, and for TEN it is 30%. The early presentation of this case makes it interesting and may give rise to future investigations of other cases with atypical presentation. Knowing the possible triggers of toxicodermias in pediatrics helps physicians not to omit or minimize the risk of this adverse reaction, regardless of its low incidence.
Author Biographies
Laura Zulema Mosquera Vilelgas, Military University Nueva Granada
Médico general, Facultad de Medicina, Universidad Militar Nueva Granada, Bogotá, Colombia.
Daniela Guevara-Parra, Hospital Universitario Clínica San Rafael, Bogotá, Colombia
Médico general, Facultad de Medicina, Universidad Militar Nueva Granada. Residente de Pediatría, Facultad de Medicina Universidad Militar Nueva Granada. Hospital Universitario Clínica San Rafael, Bogotá, Colombia.
Alejandra Granados-Betancur, Fundación Universitaria Visión de las Américas, Pereira, Colombia
Médico general, Fundación Universitaria Visión de las Américas, Pereira, Colombia.
Dilia Pinzón-Sánchez, Hospital Universitario Clínica San Rafael, Bogotá, Colombia
Especialista en Pediatría, Facultad de Medicina, Universidad Militar Nueva Granada. Pediatra, Hospital Universitario Clínica San Rafael, Bogotá, Colombia.
References
Burris Katy Schwartz Robert, Zuuren Esther, y Randall Dan, «Drug Rash With Eosinophilia and Systemic Symptoms (DRESS) Syndrome», Dynamed, vol. 38, dic. 2024, [En línea]. Disponible en: https://www.dynamed.com/condition/drug-rash-with-eosinophilia-and-systemic-symptoms-dress-syndrome
J. Bolognia, Julie Schaffer, y Lorenzo Cerroni, Fourth Edition Dermatology, vol. 2. 2017.
M.-I. A. Jimenez Rodriguez P., Toxicodermias, eritema multiforme, sindrome de stevens-johnson y necrolisis epidermica toxica. Master de Formación Permanente en Dermatología Médico-Quirúrgica y Estética. en Modulo 1: Enfermedades inflamatorias. Panamericana.
M. Ramien y J. Goldman, «Pediatric SJS - TEN: Where are we now?», Aug 2020, vol. 13, n.o 9, doi: https://doi.org/10.12688/f1000research.20419.1.
B. Abtahi-Naeini et al., «Clinical and Epidemiological Features of Patients with Drug-Induced Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in Iran: Different Points of Children from Adults», 8 Feb 2022, doi: https://doi.org/10.1155/2022/8163588.
C. Min-Hui et al., «Clinical features and outcomes in children with Stevens-Johnson syndrome and toxic epidermal necrolysis», J Dermatol, vol. 49, n.o 9, pp. 895-902, jun. 2022, doi: https://doi.org/10.1111/1346-8138.16476.
A. Pejcic et al., «Amoxicillin-associated Stevens-Johnson syndrome or toxic epidermal necrolysis: systematic review», J Chemother, vol. 35, n.o 2, pp. 75-86, mar. 2022, doi: https://doi.org/10.1080/1120009X.2022.2051128.
K. Gleghorn y C. Voigt, «Toxic epidermal necrolysis and Stevens-Johnson syndrome/toxic epidermal necrolysis overlap in pediatric patients with a focus on newer antiepileptic drugs: A 25-year retrospective study at a single tertiary care center», Pediatr Dermatol., vol. 38, n.o 4, pp. 812-818, may 2021, doi: https://doi.org/10.1111/pde.14598.
M. Ramien, «Stevens-Johnson syndrome in children», Aug 2022, vol. 1, n.o 34, pp. 341-348, doi: https://doi.org/10.1097/MOP.0000000000001146.
A. Gibson et al., «Updates on the immunopathology and genomics of severe cutaneous adverse drug reactions», Feb 2023, vol. 151, n.o 2, pp. 289-300, doi: https://doi.org/10.1016/j.jaci.2022.12.005.
How to Cite
Downloads
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Laura Zulema Mosquera Vilelgas

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.