Clinical and sociodemographic characterization of rosacea in a clinic of Manizales
DOI:
https://doi.org/10.29176/2590843X.1931Keywords:
Erythema, Prevalence, Rhinophyma, Rosacea, Telangiectasia, Epidemiology, ColombiaAbstract
Introduction: Rosacea is a chronic inflammatory skin disease with both intrinsic and environmental trig gers that manifest with various cutaneous features, such as persistent facial erythema, papules, pustules, telangiectasias, rhinophyma, ocular involvement, and facial burning or stinging sensations. It occurs mainly in women between 30 and 40 years of age, with and estimated prevalence of 5.46%. The most widely used previous classification was that based on subtypes, with erythematotelangiectatic and papulopustular being the most frequent globally. Its diagnosis is clinical, and its treatment is symptom-oriented.
Methodology: This is an observational, descriptive, retrospective, cross-sectional study. We included 247 patients of all ages, with a diagnosis of rosacea from a high-complexity healthcare institution (IPS) in Manizales. We assessed age, phototype, sex, rosacea subtype, medical history, and place of origin. Data were analyzed using OpenRefine 3.7.0 and Jamovi 2.3.21.
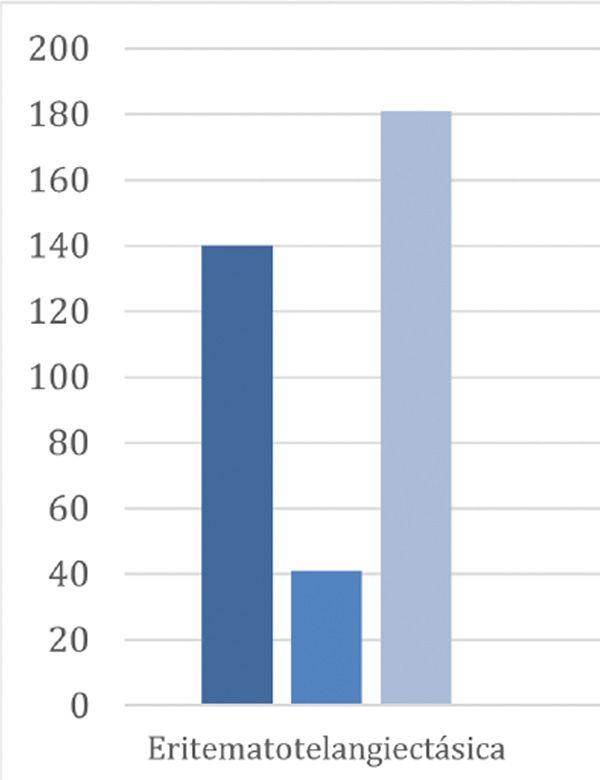
Results: A total of 247 patients were analyzed, aged between 35 and 65 years, with an average of 46.19 years. The majority were women (77.3%). The main subtype was erythematotelangiectatic (73%), followed by papulopustular (50%). The most frequent phototype was phototype III (3.6%) and phototype II (1.6%). The main comorbidity was cardiovascular disease (19%).
Conclusions: Patients with rosacea at the IPS in Manizales are predominantly women with phototypes II and III, presenting mostly with the erythematotelangiectatic subtype. Better recognition of this condition will allow for more precise therapeutic approaches, positively impacting the quality of life of those affected.
Author Biographies
Diego Mauricio Martínez Zúñiga, Universidad Libre de Colombia
Médico, dermatólogo, Universidad Libre, Cali
Stefanía García Cruz, University of Caldas
Médica, Universidad de Caldas, Manizales.
María Pineda Muñoz, University of Caldas
Médica, Universidad de Caldas, Manizales.
Paula Fandiño Rodriguez, University of Caldas
Médica, Universidad de Caldas, Manizales.
Gustavo Delgado López, University of Caldas
Médico, Universidad de Caldas, Manizales.
References
Steinhoff M, Buddenkotte J, Aubert J, et al. Clinical, cellular, and molecular aspects in the pathophysiology of rosacea. J Investig Dermatol Symp Proc. 2011;15(1):2-11. https://doi.org/10.1038/jidsymp.2011.7
Buddenkotte J, Steinhoff M. Recent advances in understanding and managing rosacea. F1000Res. 2018;7F1000 Faculty Rev-1885. https://doi. org/10.12688/f1000research.16537.1
Rosental de Kaminsky A, Piquero Mart J (editores). Rosácea: una visión integral. Ciudad Autónoma de Buenos Aires: GILER; 2018.
Reinholz M, Ruzicka T, Steinhoff M, Schaller M, Gieler U, Schöfer H, et al. Pathogenesis and clinical presentation of rosacea as a key for a symptomoriented therapy. J Ger Soc Dermatol. 2016;14(6):415.
Melnik BC. Rosacea: The Blessing of the Celts – An Approach to Pathogenesis Through Translational Research. Acta Derm Venereol. 2016;96(2):147-56. https://doi.org/10.2340/00015555-2220
Augustin M, Herberger K, Hintzen S, Heigel H, Franzke N, Schäfer I. Prevalence of skin lesions and need for treatment in a cohort of 90,880 workers. Br J Dermatol. 2011;165:865-7.
Scheinfeld N, Berk T. A Review of the Diagnosis and Treatment of Rosacea. Postgrad Med. 2010;122(1):139-43.
Azulay RD, Cañizares O, Padilla HC, Sobral C, Soto LD, Prieto JG, et al. Actualización y recomendaciones para el diagnóstico y tratamiento de la rosácea en Latinoamérica. Med Cutánea. 2016;44(s1):S7S26.
Moustafa FA, Sandoval LF, Feldman SR. Rosacea: new and emerging treatments. Drugs. 2014;74(13):1457-65. https://doi.org/10.1007/ s40265-014-0281-x
Lal Khatri M. Spectrum of skin diseases in Yemen (Hajjah and adjacent region). Int J Dermatol. 2004;43(8):580-5. https://doi.org/10.1111/j.13654632.2004.02212.x
Rueda LJ, Motta A, Pabón JG, Barona MI, Meléndez E, Orozco B, et al. Epidemiology of rosacea in Colombia. Int J Dermatol. 2017;56(5):510-3.
Bonamigo RR, Bakos L, Cartell A. Fatores associados à rosácea em amostras populacionais do sul do Brasil: análise de estudos casos-controles. An Bras Dermatol. 2008;83(5):419-4.
Gallo RL, Granstein RD, Kang S, Mannis M, Steinhoff M, Tan J, et al. Standard classification and pathophysiology of rosacea: The 2017 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol. 2018;78(1):148-55. https://doi. org/10.1016/j.jaad.2017.08.037
Barona MI, Orozco B, Motta A, Meléndez E, Rojas RF, Pabón JG, et al. Rosácea: actualización. Piel. 2015;30(8):485-502.
Egeberg A, Ashina M, Gaist D, et al. Prevalence and risk of migraine in patients with rosacea: A population- based cohort study. J Am Acad Dermatol. 2017;76(3):454-8. https://doi.org/10.1016/j. jaad.2016.08.055
Tan J, Berg M. Rosacea: current state of epidemiology. J Am Acad Dermatol. 2013;69(6 Suppl 1):S27S35. https://doi.org/10.1016/j.jaad.2013.04.043 17.
Powell FC. Clinical practice. Rosacea. N Engl J Med. 2005;352(8):793-803.
Tan J, Almeida LMC, Bewley A, Cribier B, Dlova NC, Gallo R, et al. Updating the diagnosis, classification and assessment of rosacea: recommendations from the global ROSacea COnsensus (ROSCO) panel. Br J Dermatol. 2017;176(2):431-8.
Schaefer I, Rustenbach SJ, Zimmer L, et al. Prevalence of skin dis- eases in a cohort of 48,665 employees in Germany. Dermatology. 2008;217(2):169-72. https://doi.org/10.1159/000136656
Huynh D. OpenRefine. Mountain View, CA 94042: Creative Commons Attribution 4.0 International License.; (Versión 3.7.0) [Software informático]. 2019. Disponible en: https://openrefine.org/
Selker J, Love J, Dropmann D. jmv: The ‘Jamovi’ Analyses. R package (Versión 2.3.21) [Software informático]. 2020. Disponible en: https://www.jamovi.org/
Tan J, Schöfer H, Araviiskaia E, Audibert F, Kerrouche N, Berg M, et al. Prevalence of rosacea in the general population of Germany and Russia –The RISE study. J Eur Acad Dermatol Venereol. 2016;30(3):428-34. https://doi.org/10.1111/jdv.13556
Abram K, Silm H, Oona M. Prevalence of rosacea in an Estonian working population using a standard classification. Acta Derm Venereol. 2010;90(3):26973. https://doi.org/10.2340/00015555-0856
Gutierrez EL, Galarza C, Ramos W, et al. Influence of climatic factors on the medical attentions of dermatologic diseases in a hospital of Lima, Peru. An Bras Dermatol. 2010;85(4):461-8. https://doi. org/10.1590/s0365-05962010000400007
Bae YI, Yun SJ, Lee JB, Kim SJ, Won YH, Lee SC. Clinical evaluation of 168 Korean patients with rosacea: the sun exposure correlates with the erythematotelangiectatic subtype. Ann Dermatol. 2009;21(3):243-9. https://doi.org/10.5021/ad.2009.21.3.243
Jansen T. Rosacea. En: Plewig G, Kligman A (editores). ACNE and ROSACEA. 3.a edición. Berlín, Heidelberg: Springer-Verlag; 2000. p459-65.
McAleer MA, Fitzpatrick P, Powell FC. Papulopustular rosacea: prevalence and relationship to photodamage. J Am Acad Dermatol. 2010;63(1):33-9. https://doi.org/10.1016/j.jaad.2009.04.024
Argenziano G, Donnarumma G, Iovene MR, et al. Incidence of anti-helicobacter pylori and anti-CagA antibodies in rosacea patients. Int J Dermatol. 2003;42(8):601-4. https://doi.org/10.1046/j.13654362.2003.01817.x
Egeberg A, Hansen PR, Gislasom GH, et al. Clus tering of autoinmune diseases in patients with rosacea. J Am Acad Dermatol. 2016;74(4):667-72. https://doi.org/10.1016/j.jaad.2015.11.004
Gallo RL, Granstein RD, Kang S, et al. Rosacea comorbidities and future research: The 2017 update by the National Rosacea Society Expert Committee. J Am Acad Dermatol. 2018;78(1):167-70. https://doi. org/10.1016/j.jaad.2017.06.150
Luque A, Rojas AP, Ortiz-Florez A, Perez-Bernal J. Botulinum Toxin: An Effective Treatment for Flushing and Persistent Erythema in Rosacea. J Clin Aesthet Dermatol. 2021;14(3):42-5.
How to Cite
Downloads
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Diego Mauricio Martínez Zúñiga, Stefanía García Cruz, María Pineda Muñoz, Paula Fandiño Rodriguez, Gustavo Delgado López

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |







